Clinical Study
STI Season: Understanding the Spring and Summer Surge in Healthcare Visits

Dr. Azia Evans • May 7, 2024
When we discuss the seasonality of infections, respiratory infections often come to mind. These infections follow a predictable pattern of surges and low points throughout the year, influenced by seasonal weather patterns and individual behavior changes1. However, sexually transmitted infections (STIs), skin and soft tissue infections, and urinary tract infections are not typically associated with seasonal circulation patterns. Despite the absence of the same drivers of seasonal temperature and humidity, healthcare offices, particularly urgent care facilities, which are at the forefront of diagnosing and treating most acute outpatient infections, do observe seasonal variations in the number of office visits related to these infections 2.
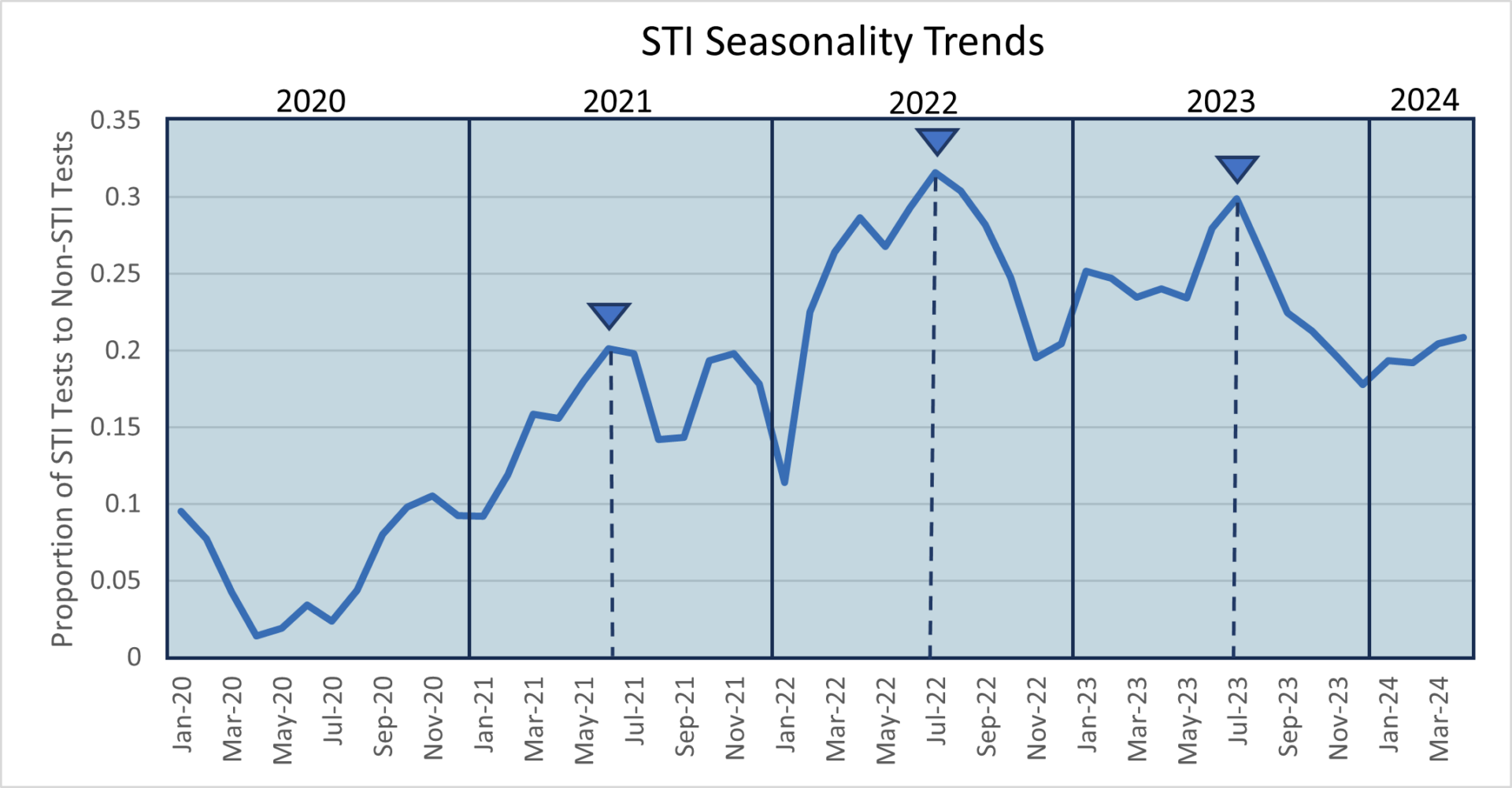
Data from 2017 published in the Journal of Urgent Care Medicine indicates that Urgent Care related visits for STIs increase throughout the spring and summer months, peaking in the early fall before dropping substantially as visits shift towards respiratory infections in the winter months. More recent data from HealthTrackRx, which looks at related laboratory tests ordered as a function of season, suggests that the proportion of STI tests compared to other infections begins to increase in the spring months, peaks in July, before decreasing throughout the fall and early winter months. This difference between 2017 and 2020-2023 is likely attributed to the changes in respiratory virus seasonality, as the last two years have shown late summer/early fall increases in both rhinovirus and COVID-19 rates. Shifting the balance of STI-related visits to respiratory visits earlier in the fall than what was seen pre-pandemic.
Drivers of STI seasonality are largely attributed to changes in human behavior and an increase in transmission contact rates that tend to peak in the warmer months. Five-year trend data from the CDC shows that between 2018 and 2022, chlamydia cases have declined, while gonorrhea and syphilis cases have been consistently on the rise3. However, when we look at one-year trend data, from 2021 to 2022, the directionality of the trends has started to flip, showing an increase in chlamydia cases, while gonorrhea cases have been on the decline.
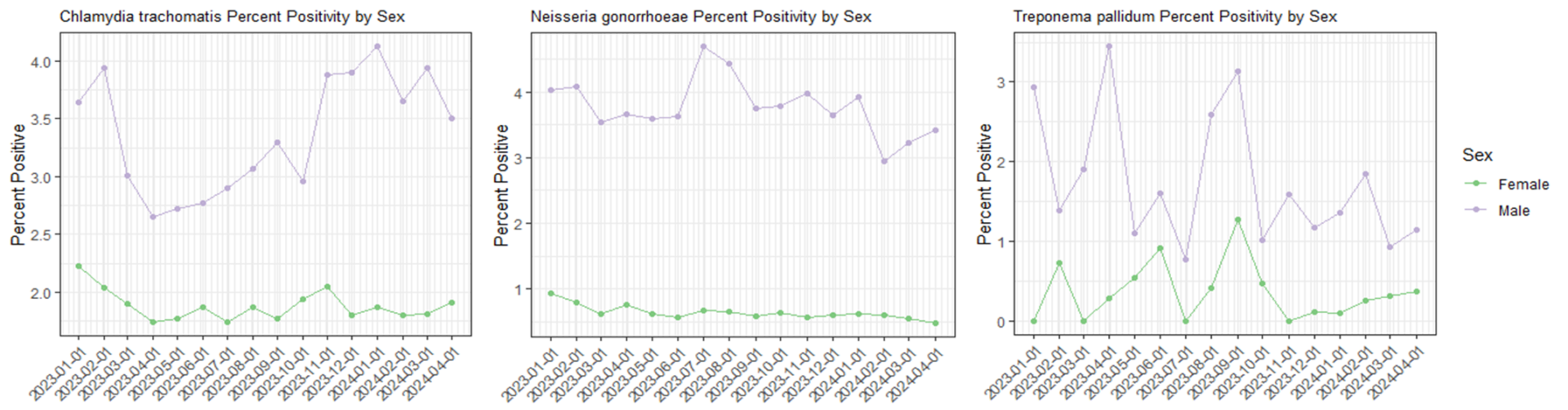
Looking more recently at 2023-2024 (YTD) positivity trend data from HealthTrackRx, chlamydia and gonorrhea cases are both substantially higher than syphilis. Although chlamydia cases are showing some fluctuation and upward trend movement, gonorrhea cases have been on a gradual decline over the past year. Notably, for all three STIs, the incidence rate in males is substantially higher than in females.
While the incidence rate and the number of healthcare-related visits for STIs continue to rise overall, the importance of rapid diagnostics for identifying these infections is critical for effective pathogen-directed treatment and patient health. If left untreated, the complications associated with undiagnosed STIs are immense, including pelvic inflammatory disease in women, increased risk of HIV, and, in certain cases, cancer or infertility. In addition, the risk of congenital infections also highlights the need for rapid and effective diagnostics. Most recently, the CDC has noted that the number of congenital syphilis cases has been steadily on the rise over the last several years4.
Current guidance advises screening of chlamydia and gonorrhea in asymptomatic sexually active female patients under the age of 25 and men who fall under the category of high-risk sexual behavior5. Screening for syphilis is only recommended in women and men who fall into the increased risk category. This is largely due to the low rates of syphilis seen over the past several decades. However, as syphilis cases continue to increase, this may also indicate a need for increased consideration of testing in patients who both present with symptoms and concerns of STI exposure.
Current STI diagnostics predominantly rely on some form of nucleic acid amplification testing (NAAT), like polymerase chain reaction (PCR). This is largely due to the increased sensitivity of these tests compared to culture and the challenges culturing both Chlamydia trachomatis and Neisseria gonorrhoeae present. In addition to improved accuracy of detection, these tests also often provide a faster time to result, leading to more effective treatment and reduced risk of spread.
STIs continue to rise, and as we head into the summer months, healthcare providers can expect to see an increase in office visits related to STI exposure. Due to the increased long-term risk to patients when STIs go undiagnosed, rapid diagnostic testing like PCR can help improve care, by getting the patient treated with the correct therapy faster and reducing the risk of missed infections due to poor diagnostic performance or low sensitivity of non-molecular-based tests.
References
- Moriyama, M., Hugentobler, W. J., & Iwasaki, A. (2020). Annual Review of Virology Seasonality of Respiratory Viral Infections. https://doi.org/10.1146/annurev-virology-012420-022445.
- Seasonality of Sexually Transmitted Infections vs Normal Urgent Care Seasonality. January 31, 2017. Journal of Urgent Care Medicine. https://www.jucm.com/seasonality-sexually-transmitted-infections-vs-normal-urgent-care-seasonality/#:~:text=With%20urgent%20care’s%20typical%20seasonality,%E2%80%9Ctypical%E2%80%9D%20urgent%20care%20volume.
- Sexually Transmitted Infections Surveillance, 2022. Centers for Disease Control and Prevention. https://www.cdc.gov/std/statistics/2022/default.htm#:~:text=Overall%2C%20in%202022%2C%20more%20than,in%20the%20past%20five%20years.
- Congenital Syphilis – CDC Fact Sheet. Centers for Disease Control and Prevention. https://www.cdc.gov/std/syphilis/stdfact-congenital-syphilis.htm.
- Sexually Transmitted Infections Treatment Guidelines, 2021: Screening Recommendations and Considerations Referenced in Treatment Guidelines and Original Sources. Centers for Disease Control and Prevention. https://www.cdc.gov/std/treatment-guidelines/screening-recommendations.htm.
References
- Moriyama, M., Hugentobler, W. J., & Iwasaki, A. (2020). Annual Review of Virology Seasonality of Respiratory Viral Infections. https://doi.org/10.1146/annurev-virology-012420-022445.
- Seasonality of Sexually Transmitted Infections vs Normal Urgent Care Seasonality. January 31, 2017. Journal of Urgent Care Medicine. https://www.jucm.com/seasonality-sexually-transmitted-infections-vs-normal-urgent-care-seasonality/#:~:text=With%20urgent%20care’s%20typical%20seasonality,%E2%80%9Ctypical%E2%80%9D%20urgent%20care%20volume.
- Sexually Transmitted Infections Surveillance, 2022. Centers for Disease Control and Prevention. https://www.cdc.gov/std/statistics/2022/default.htm#:~:text=Overall%2C%20in%202022%2C%20more%20than,in%20the%20past%20five%20years.
- Congenital Syphilis – CDC Fact Sheet. Centers for Disease Control and Prevention. https://www.cdc.gov/std/syphilis/stdfact-congenital-syphilis.htm.
- Sexually Transmitted Infections Treatment Guidelines, 2021: Screening Recommendations and Considerations Referenced in Treatment Guidelines and Original Sources. Centers for Disease Control and Prevention. https://www.cdc.gov/std/treatment-guidelines/screening-recommendations.htm.
Related Articles and White papers

Dr. Azia Evans • May 7, 2024
When we discuss the seasonality of infections, respiratory infections often come to mind. These infections follow a predictable pattern of surges and low points throughout the year, influenced by seasonal weather patterns and individual behavior changes1. However, sexually transmitted infections (STIs), skin and soft tissue infections, and urinary tract infections are not typically associated with seasonal circulation patterns. Despite the absence of the same drivers of seasonal temperature and humidity, healthcare offices, particularly urgent care facilities, which are at the forefront of diagnosing and treating most acute outpatient infections, do observe seasonal variations in the number of office visits related to these infections 2.
Data from 2017 published in the Journal of Urgent Care Medicine indicates that Urgent Care related visits for STIs increase throughout the spring and summer months, peaking in the early fall before dropping substantially as visits shift towards respiratory infections in the winter months. More recent data from HealthTrackRx, which looks at related laboratory tests ordered as a function of season, suggests that the proportion of STI tests compared to other infections begins to increase in the spring months, peaks in July, before decreasing throughout the fall and early winter months. This difference between 2017 and 2020-2023 is likely attributed to the changes in respiratory virus seasonality, as the last two years have shown late summer/early fall increases in both rhinovirus and COVID-19 rates. Shifting the balance of STI-related visits to respiratory visits earlier in the fall than what was seen pre-pandemic.

Drivers of STI seasonality are largely attributed to changes in human behavior and an increase in transmission contact rates that tend to peak in the warmer months. Five-year trend data from the CDC shows that between 2018 and 2022, chlamydia cases have declined, while gonorrhea and syphilis cases have been consistently on the rise3. However, when we look at one-year trend data, from 2021 to 2022, the directionality of the trends has started to flip, showing an increase in chlamydia cases, while gonorrhea cases have been on the decline.

Looking more recently at 2023-2024 (YTD) positivity trend data from HealthTrackRx, chlamydia and gonorrhea cases are both substantially higher than syphilis. Although chlamydia cases are showing some fluctuation and upward trend movement, gonorrhea cases have been on a gradual decline over the past year. Notably, for all three STIs, the incidence rate in males is substantially higher than in females.
While the incidence rate and the number of healthcare-related visits for STIs continue to rise overall, the importance of rapid diagnostics for identifying these infections is critical for effective pathogen-directed treatment and patient health. If left untreated, the complications associated with undiagnosed STIs are immense, including pelvic inflammatory disease in women, increased risk of HIV, and, in certain cases, cancer or infertility. In addition, the risk of congenital infections also highlights the need for rapid and effective diagnostics. Most recently, the CDC has noted that the number of congenital syphilis cases has been steadily on the rise over the last several years4.
Current guidance advises screening of chlamydia and gonorrhea in asymptomatic sexually active female patients under the age of 25 and men who fall under the category of high-risk sexual behavior5. Screening for syphilis is only recommended in women and men who fall into the increased risk category. This is largely due to the low rates of syphilis seen over the past several decades. However, as syphilis cases continue to increase, this may also indicate a need for increased consideration of testing in patients who both present with symptoms and concerns of STI exposure.
Current STI diagnostics predominantly rely on some form of nucleic acid amplification testing (NAAT), like polymerase chain reaction (PCR). This is largely due to the increased sensitivity of these tests compared to culture and the challenges culturing both Chlamydia trachomatis and Neisseria gonorrhoeae present. In addition to improved accuracy of detection, these tests also often provide a faster time to result, leading to more effective treatment and reduced risk of spread.
STIs continue to rise, and as we head into the summer months, healthcare providers can expect to see an increase in office visits related to STI exposure. Due to the increased long-term risk to patients when STIs go undiagnosed, rapid diagnostic testing like PCR can help improve care, by getting the patient treated with the correct therapy faster and reducing the risk of missed infections due to poor diagnostic performance or low sensitivity of non-molecular-based tests.
References
- Moriyama, M., Hugentobler, W. J., & Iwasaki, A. (2020). Annual Review of Virology Seasonality of Respiratory Viral Infections. https://doi.org/10.1146/annurev-virology-012420-022445.
- Seasonality of Sexually Transmitted Infections vs Normal Urgent Care Seasonality. January 31, 2017. Journal of Urgent Care Medicine. https://www.jucm.com/seasonality-sexually-transmitted-infections-vs-normal-urgent-care-seasonality/#:~:text=With%20urgent%20care’s%20typical%20seasonality,%E2%80%9Ctypical%E2%80%9D%20urgent%20care%20volume.
- Sexually Transmitted Infections Surveillance, 2022. Centers for Disease Control and Prevention. https://www.cdc.gov/std/statistics/2022/default.htm#:~:text=Overall%2C%20in%202022%2C%20more%20than,in%20the%20past%20five%20years.
- Congenital Syphilis – CDC Fact Sheet. Centers for Disease Control and Prevention. https://www.cdc.gov/std/syphilis/stdfact-congenital-syphilis.htm.
- Sexually Transmitted Infections Treatment Guidelines, 2021: Screening Recommendations and Considerations Referenced in Treatment Guidelines and Original Sources. Centers for Disease Control and Prevention. https://www.cdc.gov/std/treatment-guidelines/screening-recommendations.htm.
References
- Moriyama, M., Hugentobler, W. J., & Iwasaki, A. (2020). Annual Review of Virology Seasonality of Respiratory Viral Infections. https://doi.org/10.1146/annurev-virology-012420-022445.
- Seasonality of Sexually Transmitted Infections vs Normal Urgent Care Seasonality. January 31, 2017. Journal of Urgent Care Medicine. https://www.jucm.com/seasonality-sexually-transmitted-infections-vs-normal-urgent-care-seasonality/#:~:text=With%20urgent%20care’s%20typical%20seasonality,%E2%80%9Ctypical%E2%80%9D%20urgent%20care%20volume.
- Sexually Transmitted Infections Surveillance, 2022. Centers for Disease Control and Prevention. https://www.cdc.gov/std/statistics/2022/default.htm#:~:text=Overall%2C%20in%202022%2C%20more%20than,in%20the%20past%20five%20years.
- Congenital Syphilis – CDC Fact Sheet. Centers for Disease Control and Prevention. https://www.cdc.gov/std/syphilis/stdfact-congenital-syphilis.htm.
- Sexually Transmitted Infections Treatment Guidelines, 2021: Screening Recommendations and Considerations Referenced in Treatment Guidelines and Original Sources. Centers for Disease Control and Prevention. https://www.cdc.gov/std/treatment-guidelines/screening-recommendations.htm.
Related Articles and White papers