NOT EVERY BUG NEEDS A DRUG
Understanding antibiotic resistance—and why the right test matters.
Antibiotics save lives when used correctly. But not all infections respond to them and using antibiotics when they’re not needed can make them stop working when it matters most. It’s time to make sure you get the right care at the right time.
NOT EVERY BUG NEEDS A DRUG
Understanding antibiotic resistance—and why the right test matters.
Antibiotics save lives when used correctly. But not all infections respond to them and using antibiotics when they’re not needed can make them stop working when it matters most. It’s time to make sure you get the right care at the right time.
What Is Antibiotic Resistance?
Antibiotic resistance means that germs (certain bacteria) have changed in a way that makes the antibiotics we use to kill them no longer work.
Here’s a simple way to think about it:
- Antibiotics are medicines that kill bacteria.
- Bacteria are tiny organisms that can cause infections.
- Over time, some bacteria learn to survive even when antibiotics try to kill them.
- These tough bacteria can adapt and spread, making infections harder to treat.
Important: Antibiotic resistance doesn’t mean your body is resistant. It means the bacteria have become stronger, and our medicines aren’t as effective as before.
41% of Americans falsely believe antibiotics can treat illnesses caused by viruses. Antibiotics only work on bacterial infections. They don’t work on viral infections like the common cold, flu or COVID-19. That’s why testing matters—to know what’s causing your symptoms.
What Is Antibiotic Resistance?
Antibiotic resistance means that germs (certain bacteria) have changed in a way that makes the antibiotics we use to kill them no longer work.
Here’s a simple way to think about it:
- Antibiotics are medicines that kill bacteria.
- Bacteria are tiny organisms that can cause infections.
- Over time, some bacteria learn to survive even when antibiotics try to kill them.
- These tough bacteria can adapt and spread, making infections harder to treat.
Important: Antibiotic resistance doesn’t mean your body is resistant. It means the bacteria have become stronger, and our medicines aren’t as effective as before.
41% of Americans falsely believe antibiotics can treat illnesses caused by viruses. Antibiotics only work on bacterial infections. They don’t work on viral infections like the common cold, flu or COVID-19. That’s why testing matters—to know what’s causing your symptoms.
This Affects Everyone
Antibiotic resistance isn’t an individual issue—it’s a global health threat that impacts us all.

Common infections can become dangerous Antibiotic resistance can turn minor infections into severe or even life-threatening conditions. It can also complicate childbirth, surgery, and cancer treatment.
Resistance spreads everywhere Resistance spreads between people, communities, animals, and even our environment. That means someone’s misuse of antibiotics can have far-reaching consequences, including infections that don’t respond to treatment.
Few new antibiotics are coming There are very few new classes of antibiotics developed in the last decade. If we lose the antibiotics we have now, we may not get replacements.
SEE HOW WE’RE FIGHTING BACKThis Affects Everyone
Antibiotic resistance isn’t an individual issue—it’s a global health threat that impacts us all.

Common infections can become dangerous Antibiotic resistance can turn minor infections into severe or even life-threatening conditions. It can also complicate childbirth, surgery, and cancer treatment.
Resistance spreads everywhere Resistance spreads between people, communities, animals, and even our environment. That means someone’s misuse of antibiotics can have far-reaching consequences, including infections that don’t respond to treatment.
Few new antibiotics are coming There are very few new classes of antibiotics developed in the last decade. If we lose the antibiotics we have now, we may not get replacements.
SEE HOW WE’RE FIGHTING BACKWhy Is This Happening?
Misuse and Overuse of Antibiotics
Antibiotic resistance happens when antibiotics are used incorrectly or too often. This includes:
- Not finishing your antibiotic prescription as directed
- Stopping antibiotics early when you feel better
- Saving leftover antibiotics for later use
- Taking antibiotics prescribed for someone else
- Prescribing antibiotics “just in case” when testing isn’t available quickly enough
- Responding to patient pressure for immediate treatment
- Treating viral infections (which don’t respond to antibiotics) with antibiotics

of adults admitted in a 2024 study, they would stop taking antibiotics once they felt better rather than complete the course, even though they recognized it was important to finish.
Why Is This Happening?
Misuse and Overuse of Antibiotics
Antibiotic resistance happens when antibiotics are used incorrectly or too often. This includes:
On the patient side:
- Not finishing your antibiotic prescription as directed
- Stopping antibiotics early when you feel better
- Saving leftover antibiotics for later use
- Taking antibiotics prescribed for someone else
On the healthcare side:
- Prescribing antibiotics “just in case” when testing isn’t available quickly enough
- Responding to patient pressure for immediate treatment
- Treating viral infections (which don’t respond to antibiotics) with antibiotics

The Numbers Tell the Story
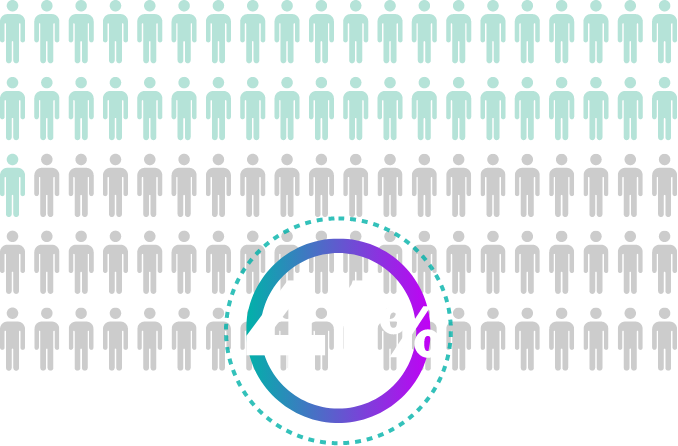
falsely believe antibiotics can treat viral illness
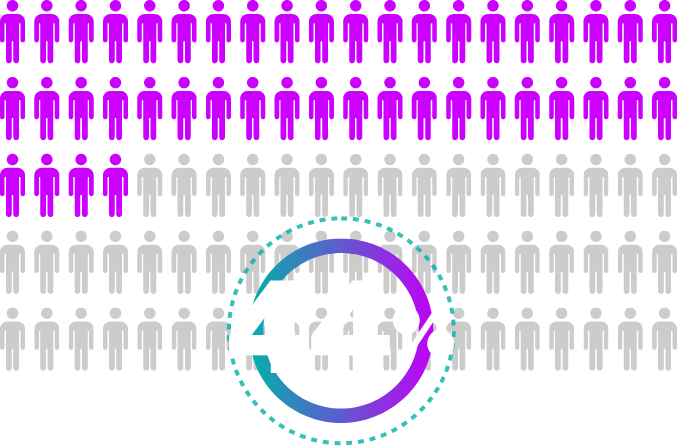
have been prescribed antibiotics two or more times in the past five years

say their most recent antibiotic prescription was given without testing
of outpatient antibiotics are prescribed unnecessarily1
medication-related ER visits is from antibiotic side effects.3
The estimated cost to treat Americans with infections caused by antimicrobial-resistant germs.4
resistant infections in the U.S. annually.2
Americans die yearly from antimicrobial-resistant infections.2
By 2050:
The toll of drug-resistant infections is predicted to rise by 70%, leading to significant loss of life.5
deaths globally each year5

deaths in the U.S. each year5
*12/25 HealthTrack VoC Survey
1 Hersh AL, King LM, Shapiro DJ, Hicks LA, Fleming-Dutra KE. Unnecessary Antibiotic Prescribing in US Ambulatory Care Settings, 2010-2015. Clinical Infectious Diseases. 2021;72(1):133-137.
2 Centers for Disease Control and Prevention. (2025). Antimicrobial resistance: Causes and how it spreads.
3 Shehab N, Lovegrove MC, Geller AI, et al. US emergency department visits for outpatient adverse drug events, 2013-2014. JAMA. 2016;316(20):2115-2125.
4 Nelson, R. E., Hatfield, K. M., Wolford, H., et al. (2021). National estimates of healthcare costs associated with multidrug-resistant bacterial infections among hospitalized patients in the United States. Clinical Infectious Diseases, 72(Suppl 1), S17-S26.
5 Nature. 40 million deaths by 2050: Toll of drug-resistant infections to rise by 70%.
The Numbers Tell the Story

falsely believe antibiotics can treat viral illness

have been prescribed antibiotics two or more times in the past five years

say their most recent antibiotic prescription was given without testing
of outpatient antibiotics are prescribed unnecessarily1
medication-related ER visits is from antibiotic side effects.3
The estimated cost to treat Americans with infections caused by antimicrobial-resistant germs.4
resistant infections in the U.S. annually.2
Americans die yearly from antimicrobial-resistant infections.2

By 2050:
The toll of drug-resistant infections is predicted to rise by 70%, leading to significant loss of life.5
deaths globally each year5
deaths in the U.S. each year5
*12/25 HealthTrack VoC Survey
1 Hersh AL, King LM, Shapiro DJ, Hicks LA, Fleming-Dutra KE. Unnecessary Antibiotic Prescribing in US Ambulatory Care Settings, 2010-2015. Clinical Infectious Diseases. 2021;72(1):133-137.
2 Centers for Disease Control and Prevention. (2025). Antimicrobial resistance: Causes and how it spreads.
3 Shehab N, Lovegrove MC, Geller AI, et al. US emergency department visits for outpatient adverse drug events, 2013-2014. JAMA. 2016;316(20):2115-2125.
4 Nelson, R. E., Hatfield, K. M., Wolford, H., et al. (2021). National estimates of healthcare costs associated with multidrug-resistant bacterial infections among hospitalized patients in the United States. Clinical Infectious Diseases, 72(Suppl 1), S17-S26.
5 Nature. 40 million deaths by 2050: Toll of drug-resistant infections to rise by 70%.
The Solution:
Smarter Testing Leads to Better Care
Healthtrack provides fast, accurate answers that help your provider know when antibiotics are truly needed.
The Solution:
Smarter
Testing Leads
to Better Care
Healthtrack provides fast, accurate answers that help your provider know when antibiotics are truly needed.
Ask Your Provider for Healthtrack PCR Testing
Healthtrack provides Polymerase Chain Reaction (PCR) testing that gives your provider fast, accurate information about what’s causing your infection. PCR testing uses genetic material (DNA) to better analyze a test sample.
With next-morning PCR results, your provider can:
- Identify the exact pathogen causing your symptoms
- Next-morning clarity enables guideline-based treatment and naturally supports stewardship.
- Make informed decisions based on science, not guesswork
- Prescribe the right treatment the first time
This means fewer unnecessary antibiotics, better outcomes, and protection against “superbugs” (bacteria that no longer respond to antibiotics).
Why your provider might not prescribe an antibiotic right away: If your provider wants to run tests before prescribing antibiotics, that’s a good thing. They’re using diagnostic findings to have a shared decision-making conversation with you. This approach prevents antibiotic misuse, which helps combat resistance—a growing public health crisis. It also allows you to receive the right care by the next morning after your appointment.
Ask Your Provider for Healthtrack PCR Testing
Healthtrack provides Polymerase Chain Reaction (PCR) testing that gives your provider fast, accurate information about what’s causing your infection. PCR testing uses genetic material (DNA) to better analyze a test sample.
With next-morning PCR results, your provider can:
- Identify the exact pathogen causing your symptoms
- Next-morning clarity enables guideline-based treatment and naturally supports stewardship.
- Make informed decisions based on science, not guesswork
- Prescribe the right treatment the first time
This means fewer unnecessary antibiotics, better outcomes, and protection against “superbugs” (bacteria that no longer respond to antibiotics).
Why your provider might not prescribe an antibiotic right away: If your provider wants to run tests before prescribing antibiotics, that’s a good thing. They’re using diagnostic findings to have a shared decision-making conversation with you. This approach prevents antibiotic misuse, which helps combat resistance—a growing public health crisis. It also allows you to receive the right care by the next morning after your appointment.
Data is based on 04/2025 HealthTrackRx VoC Survey. Respondents include over 700 MDs, PAs and NPs within urgent care, primary care, women’s health and pediatric practices.

Proven Results for Better Patient Care
We Are Evolving Antibiotic Prescribing

Patient Satisfaction Is Improving

Data is based on 04/2025 HealthTrackRx VoC Survey. Respondents include over 700 MDs, PAs and NPs within urgent care, primary care, women’s health and pediatric practices.
Proven Results for Better Patient Care


We Are Evolving Antibiotic Prescribing

Patient Satisfaction Is Improving

When Can Antibiotic Stewardship Impact You?
Clinicians who practice antibiotic stewardship take extra steps to ensure you receive accurate treatment for infectious diseases, including the right drug, dose, duration and only when needed.
Your provider may run tests or ask more questions before prescribing antibiotics in these situations:
When you might have a viral infection
Symptoms caused by viruses like COVID-19, flu, RSV, or the common cold won’t respond to antibiotics. Testing helps confirm what’s causing your illness.
When confirming a bacterial infection
Before prescribing antibiotics, your provider wants to make sure bacteria are actually causing your symptoms.
When symptoms don’t improve or come back
If you’ve been sick for a while or symptoms return, more careful testing helps identify the right treatment approach.
When you’re at greater risk
Children, older adults, pregnant women, and people with weaker immune systems benefit most from precise diagnosis and targeted treatment.
When Can Antibiotic Stewardship Impact You?
Clinicians who practice antibiotic stewardship take extra steps to ensure you receive accurate treatment for infectious diseases, including the right drug, dose, duration and only when needed.
Your provider may run tests or ask more questions before prescribing antibiotics in these situations:
When you might have a viral infection
Symptoms caused by viruses like COVID-19, flu, RSV, or the common cold won’t respond to antibiotics. Testing helps confirm what’s causing your illness.
When confirming a bacterial infection
Before prescribing antibiotics, your provider wants to make sure bacteria are actually causing your symptoms.
When symptoms don’t improve or come back
If you’ve been sick for a while or symptoms return, more careful testing helps identify the right treatment approach.
When you’re at greater risk
Children, older adults, pregnant women, and people with weaker immune systems benefit most from precise diagnosis and targeted treatment.
Learn More About Your Health
Explore our patient education resources on common infections and testing.
Learn More
About Your
Health
Explore our patient education resources on common infections and testing.
STI Testing:
Protecting Your Sexual Health